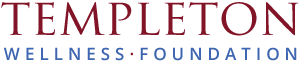When I was diagnosed with Stage IV Melanoma over 37 years ago, my world fell apart in ways I could never have imagined. Hearing those three dreaded words, “You have cancer,” that put it all in motion, is something I can never forget. My journey back to health was filled with twists and turns, but I can say from my vantage point today, that the devastating diagnosis I received back then was eventually transformed into a powerful story of resilience, hope, and triumph over adversity. If I can do it, then why can’t you? You just have to role up your sleeves and get busy.
Thankfully, today I am not only healthy and cancer-free, I am also passionately committed to sharing my journey and inspiring others to explore the many alternative options for cancer care. Through The Templeton Wellness Foundation, my aim is to offer hope and knowledge while leading people towards holistic approaches that foster healing and well-being.
Understanding Melanoma
Skin cancer is a widespread and common form of cancer, with melanomas being one of its more dangerous forms. According to the World Cancer Research Fund, Melanoma skin cancer is the 13th most common cancer in men and the 15th most common cancer in women. There were more than 150,000 new cases of melanoma of skin in 2020.
Melanoma is a cancer characterized by uncontrollable growth of melanocytes – cells which produce melanin, the pigment responsible for coloring our skin, hair and eyes – without control from their natural regulators (melanocytes). Although most commonly seen on areas exposed to sunlight such as faces, necks, arms or legs; it can also develop on soles of feet palms of hands and under nails where minimal sunlight exposure exists.
Signs and Symptoms of Melanoma
The ABCDE rule can be helpful in the early detection of melanomas:
- Asymmetry: Occurs when one half of a mole or pigmented spot doesn’t align with its other half.
- Border: Moles often have irregular, blurry, or poorly defined borders.
- Color: Moles can have various shades of brown, black, red, white and blue colors within them that do not conform with uniform color schemes.
- Diameter: If the mole is greater than 6mm in size (roughly equivalent to the diameter of a pencil eraser), it may warrant further care and monitoring.
- Evolving: Moles that change their size, shape, color or exhibit symptoms like itching, bleeding or crusting should be monitored closely as these may indicate changes.
All that said, it’s important to note that not all melanomas follow these guidelines. That’s why any suspicious or changing spot should be examined by a healthcare provider immediately.
The Stages of Melanoma Progression
Melanoma progresses through various stages, each representing its growth and potential spread. These include:
- Stage 0 melanoma occurs only in the outermost skin layer, known as the epidermis.
- Stage I indicates that cancer has spread beyond this initial layer but has not metastasized to nearby lymph nodes.
- Stage II tumors tend to be larger, with increased risk of spreading to nearby lymph nodes.
- In Stage III, melanoma has spread to nearby lymph nodes or tissues but not distant organs yet.
- By Stage IV it has metastasized, spreading across organs or lymph nodes distantly.
Early diagnosis is key for treating melanoma at its early stages when it is more likely to be curable.
Risk Factors
A number of risk factors increase an individual’s chances of developing melanoma. These may include:
- The Impact of UV Rays: prolonged or intensive exposure to ultraviolet (UV) rays from the sun or tanning beds.
- Fair Skin and Vulnerability to UV Radiation: fair skin with less melanin provides less natural protection from UV radiation.
- Family History: Genetic Link to Melanoma Risk. If melanoma runs in your family, it can increase your risk of developing the disease. Understanding your family’s medical history can help assess your genetic predisposition to melanoma.
- Moles and Melanoma: multiple moles on your body, particularly ones with abnormal or dysplastic features, increases your risk.
- Age and Melanoma: Risk Factors with Time. While melanoma can affect individuals of any age, its risk rises with age.
- Prevention and Early Detection: The Power of Skin Examinations. Regular skin exams may detect early-stage cancers before symptoms arise, and preventative strategies could lower this risk even more effectively than ever before.
Preventive Steps to Take
- Avoid tanning beds: Artificial UV radiation increases the risk of melanomas.
- Perform self-examinations: Conduct regular skin checks to detect changes, and report any moles or lesions suspected as suspect to your healthcare provider immediately.
- Eat a healthy diet. Avoid sugar, grains, dairy, processed foods, and unhealthy fats. Enjoy plenty of organically-grown produce and learn which foods are ideal for fighting cancer in my article, “Fill Your Plate with These Cancer-Fighting Foods.”
- Always be sure your drinking water is filtered and as pure as possible. Why? Researchers have concluded that water contamination is likely responsible for 100,000+ cases of cancer annually here in the U.S. Read more in this article.
- Eat at home as much as you can so that you have total control over the things you eat. If you must dine out, check out The Templeton List, a resource for finding the healthiest restaurant options in your area.
- Get tested for parasites. When I met with Dr. Hermann Bueno, a world-renowned Columbian parasitologist, I’ll never forget what he said to me. Learn more in this article: The Parasite-Cancer Connection.
- Be sure to take adequate amounts of Vitamin C. Learn how Vitamin C can stop cancer in its tracks.
- Limit your exposure to dangerous toxins, and learn to detoxify your body.
- Eradicate toxic mold from your environment. I fought a battle with mold, and it’s something you don’t want to mess with. Here’s what I did: The Silent Menace of Mold and Its Related Cancer Risk
- Reduce your exposure to EMF radiation. This can be a hard one to fight, as EMF exposure is almost everywhere. But here are some steps you can take to mitigate your exposure to this deadly toxin. THIS Many Minutes on Your Smart Phone Increases Your Risk of Cancer By A Whopping 60%.
These are but a few of the steps you can take to reduce your risk of skin cancer. You can read all about my journey back to health and the many things I did to dig my way out of Stage IV melanoma in my book, I Used to Have Cancer. I also included a section on what measures I would take if I had to do it all over again.
I won’t kid you. Melanoma is no joke. If you find yourself diagnosed with this deadly form of skin cancer, waste no time in exploring all your options. Please check out the wide expanse of information on The Templeton Wellness Foundation website. You’ll find a wealth of in-depth video interviews with many of the leading healthcare experts from around the world. It’s the next best thing to sitting face to face with these cancer experts and having all your questions answered.
And you’ll also find a rich cache of some of the most inspiring cancer survivor stories you’ll ever hear. These are people just like you who fought and won their fight against cancer. And if they can do it, you can, too!
Resources:
Gandini S, Sera F, Cattaruzza MS, Pasquini P, Picconi O, Boyle P, Melchi CF. Meta-analysis of risk factors for cutaneous melanoma: II. Sun exposure. Eur J Cancer. 2005 Jan;41(1):45-60. doi: 10.1016/j.ejca.2004.10.016. PMID: 15617990.
Cust AE, Goumas C, Vuong K, Davies JR, Barrett JH, Holland EA, Schmid H, Agha-Hamilton C, Armstrong BK, Kefford RF, Aitken JF, Giles GG, Bishop D, Newton-Bishop JA, Hopper JL, Mann GJ, Jenkins MA. MC1R genotype as a predictor of early-onset melanoma, compared with self-reported and physician-measured traditional risk factors: an Australian case-control-family study. BMC Cancer. 2013 Sep 4;13:406. doi: 10.1186/1471-2407-13-406. PMID: 24134749; PMCID: PMC3766240.
Laskar R, Ferreiro-Iglesias A, Bishop DT, Iles MM, Kanetsky PA, Armstrong BK, Law MH, Goldstein AM, Aitken JF, Giles GG; Australian Melanoma Family Study Investigators; Leeds Case-Control Study Investigators; Robbins HA, Cust AE. Risk factors for melanoma by anatomical site: an evaluation of aetiological heterogeneity. Br J Dermatol. 2021 Jun;184(6):1085-1093. doi: 10.1111/bjd.19705. Epub 2021 Feb 18. PMID: 33270213; PMCID: PMC9969114.