I don’t know if you’ve ever had a live blood analysis, but if you haven’t, I encourage you to do so. It’s quite interesting. A single drop of blood, examined with the help of a darkfield microscope, is used to observe live blood cells. This unique form of blood analysis provides additional details to your medical history by highlighting nutritional deficiencies or abnormalities that could signal something is amiss in the bloodstream.
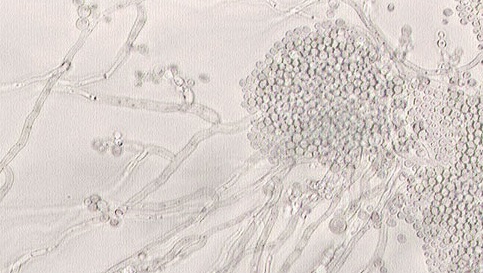
I was personally certified in microscopy and methodology by Dr. Robert Bradford in the mid-1990s. Years ago, when I saw clients, over half presented with either an overgrowth of Candida or systemic Candida — as evidenced by live blood analyses under my highly specialized Bradford microscope. Candida doesn’t act like other fungi; instead, it clusters together much like little grapes and is easy to recognize under such a powerful microscope. Of the clients I saw, those struggling with cancer or AIDS had especially elevated Candida levels. I once performed a live blood analysis on a Canadian medical doctor with AIDS who had more Candida than any person I’d ever seen before.
I am not the only one, of course, to notice the connection between Candida and cancer. Researchers have been investigating the link between this very common fungus and cancer for a long time. Emerging scientific research indicates that it is Candida’s overgrowth that is particularly concerning. Why? An overgrowth of this fungus may contribute to chronic inflammation, cause DNA damage, exude dangerous mycotoxins, and trigger the onset of cancer.
Check out my video interview with Dr. Tullio Simoncini, an oncologist from Rome, Italy. He believes cancer is caused by a fungus, namely Candida albicans.
The Fungus Among Us
Candida albicans typically coexists in harmony with other microorganisms within our body and plays an essential role in maintaining homeostasis. But the problem occurs when an imbalance arises and Candida overgrowth occurs. That’s when serious health issues may manifest.
According to research published in the Journal of Fungi, Candida species are estimated to cause over 400,000 cases of systemic fungal disease each year. Candidiasis can manifest in various forms including oral thrush, vaginal infections, and digestive disturbances. Factors that often trigger candidiasis include an impaired immune system, hormonal imbalances, prolonged antibiotic usage, or poor diet choices.
For example, you may not realize that your sweet tooth is not just satisfying your taste buds, but is providing Candida with the fuel it needs to survive – and these live organisms are causing you to crave more and more sugar. This creates a vicious cycle – crave sugar, eat sugar, feed the yeast, cause yeast to grow, — resulting in even more sugar cravings (A Path to Natural Health).
Candidiasis and Chronic Inflammation: A Potentially Dangerous Mix
Chronic inflammation has long been recognized as a risk factor for various diseases, including cancer. Recently, however, research has shed light on an association between Candida overgrowth and chronic inflammation; specifically, when excessive yeast proliferation activates an immune response leading to chronic inflammation in various parts of the body. It’s the proverbial “fuel to the fire” scenario.
Sustained inflammation creates an environment which is conducive to DNA damage, tissue destruction, and an increase in cancer risks. While more research needs to be conducted in order to understand this connection fully, emerging evidence shows the significance of maintaining an ideal balance of Candida in order to lower risks related to chronic inflammation and its potential implication for cancer development.
Candida and DNA Damage: Uncovering Molecular Clues
If you need a reason to keep Candida in check, this is it. One of the fascinating aspects of the Candida-cancer link is its potential to cause DNA damage. Persistent overgrowth of Candida can cause extensive tissue damage that eventually results in genetic mutations. These mutations may interfere with normal cell processes that regulate growth and division, increasing the risk of cancer development. Studies have identified correlations between Candida overgrowth and genetic abnormalities in tissues affected by its overgrowth, and genetic mutations associated with cancer formation, giving us preliminary insights into its cause-and-effect relationship. Yet further investigation needs to take place before any definitive causal relationships can be determined.
Mycotoxins: Candida’s Potentially Harmful Arsenal
Candida’s arsenal also includes mycotoxins – toxic substances produced by certain fungi. Mycotoxins have been known to disrupt cell functions and lower immune responses. Furthermore, mycotoxins released by Candida have the ability to not only damage DNA, but may compromise our body’s natural defense mechanisms against the development of cancer. Their presence highlights the necessity of managing Candida overgrowth to minimize health risks and mitigate future development of cancerous tumors.
The adverse health effects of mycotoxins range from acute poisoning to long-term effects such as immune deficiency and, yes, even cancer (World Health Organization).
Candida as One Piece of Cancer’s Complex Development Puzzle
An overgrowth of Candida involves multiple factors that combine genetic predisposition, lifestyle factors, environmental exposures, and coexisting health conditions that all come into play when creating an ideal environment for cancer to form. Acknowledging all these interplaying components is necessary in understanding its complexities as well as developing effective prevention and treatment strategies.
While research into the link between Candida albicans and cancer remains ongoing, preliminary evidence points towards intriguing associations. Candida overgrowth can contribute to chronic inflammation, DNA damage, and production of mycotoxins that pose risks of cancer. All three can increase chronic inflammation and lead to cancer risk.
Of course, we know that cancer development involves multiple factors and influences. Maintaining a balanced and healthy lifestyle – including proper diet and immunity support — remains key to overall wellbeing. As scientists unravel more of Candida and its possible link with cancer, future insights may provide invaluable guidance towards living healthier, cancer-free lives.
NOTE: Please keep in mind that the information provided in this article is intended as an educational source and should not be considered medical advice. For personalized guidance and treatment solutions, it is always advisable to seek guidance from your personal healthcare provider.
Related:
The Baking Soda Solution to Cancer (a video interview with Dr. Tullio Simoncini, an oncologist from Rome, Italy. He believes cancer is caused by a fungus, namely Candida albicans)
Does Fungus Cause Cancer, Or Is Cancer A Fungus? (a video interview with Doug Kaufmann, expert on the fungal connection to many infections and ailments — including heart disease, autoimmune illness, and cancer)
Resources:
Talapko J, Juzbašić M, Matijević T, Pustijanac E, Bekić S, Kotris I, Škrlec I. Candida albicans-The Virulence Factors and Clinical Manifestations of Infection. J Fungi (Basel). 2021 Jan 22;7(2):79. doi: 10.3390/jof7020079. PMID: 33499276; PMCID: PMC7912069.
Ho J, Camilli G, Griffiths JS, Richardson JP, Kichik N, Naglik JR. Candida albicans and candidalysin in inflammatory disorders and cancer. Immunology. 2021 Jan;162(1):11-16. doi: 10.1111/imm.13255. Epub 2020 Sep 13. PMID: 32880925; PMCID: PMC7730014.
Wisplinghoff H, Bischoff T, Tallent SM, Seifert H, Wenzel RP, Edmond MB. Nosocomial bloodstream infections in US hospitals: analysis of 24,179 cases from a prospective nationwide surveillance study. Clin Infect Dis. 2004 Aug 1;39(3):309-17. doi: 10.1086/421946. Epub 2004 Jul 15. Erratum in: Clin Infect Dis. 2004 Oct 1;39(7):1093. Erratum in: Clin Infect Dis. 2005 Apr 1;40(7):1077. PMID: 15306996.
Pappas PG, Rex JH, Lee J, Hamill RJ, Larsen RA, Powderly W, Kauffman CA, Hyslop N, Mangino JE, Chapman S, Horowitz HW, Edwards JE, Dismukes WE; NIAID Mycoses Study Group. A prospective observational study of candidemia: epidemiology, therapy, and influences on mortality in hospitalized adult and pediatric patients. Clin Infect Dis. 2003 Sep 1;37(5):634-43. doi: 10.1086/376906. Epub 2003 Aug 14. PMID: 12942393.
Dohlman AB, Klug J, Mesko M, Gao IH, Lipkin SM, Shen X, Iliev ID. A pan-cancer mycobiome analysis reveals fungal involvement in gastrointestinal and lung tumors. Cell. 2022 Sep 29;185(20):3807-3822.e12. doi: 10.1016/j.cell.2022.09.015. PMID: 36179671; PMCID: PMC9564002.
Wang X, Zhang W, Wu W, Wu S, Young A, Yan Z. Is Candida albicans a contributor to cancer? A critical review based on the current evidence. Microbiol Res. 2023 Jul;272:127370. doi: 10.1016/j.micres.2023.127370. Epub 2023 Mar 30. PMID: 37028206.
Shokohi T, Aslani N, Ahangarkani F, Meyabadi MF, Hagen F, Meis JF, Boekhout T, Kolecka A, Badali H. Candida infanticola and Candida spencermartinsiae yeasts: Possible emerging species in cancer patients. Microb Pathog. 2018 Feb;115:353-357. doi: 10.1016/j.micpath.2017.12.069. Epub 2017 Dec 29. PMID: 29292174.

